
Read Time: 3 minutes
A patient came in last week convinced she had sciatica.
She was having sharp pain that started in her hip and ran down her leg to her foot. Naturally, she assumed it was coming from her low back.
But it wasn’t.
What It Actually Was
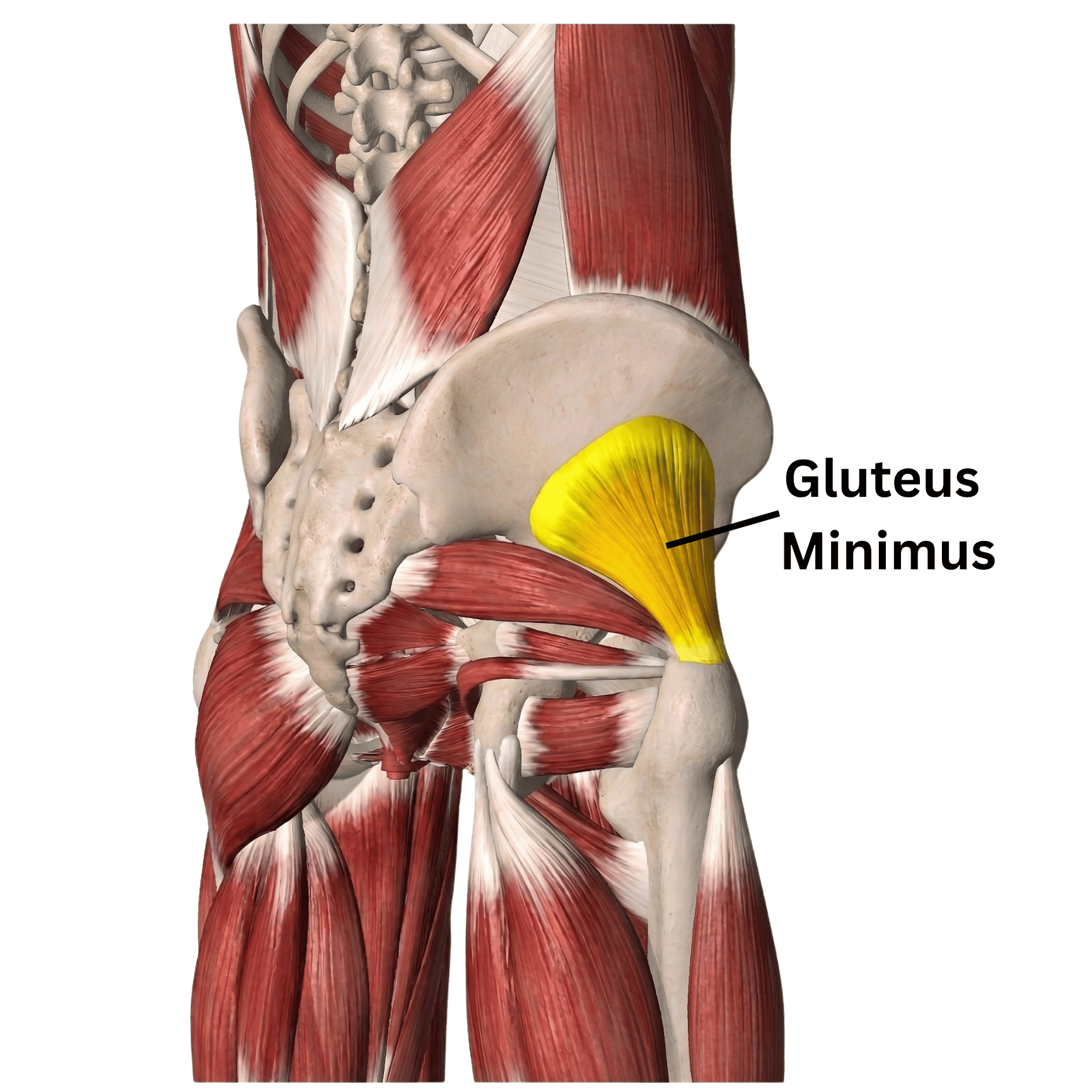
The source of her pain was a muscle in her hip called the gluteus minimus.
This muscle sits deep on the side of your hip, and when it gets irritated, it can refer pain down the side of your leg (sometimes as far as the calf or even the foot).
It can feel almost identical to sciatica, which is why people often get confused.
I’ll sometimes call it “side-atica” because of how similar it feels, even though it’s not coming from the sciatic nerve.
Why This Happens
This is more common than most people realize.
In many cases, it builds up over time from things like sitting a lot, weak glutes, or starting a new activity (like pickleball).
Essentially what happens is the glute minimus ends up doing more work than it can handle.
This causes trigger point(s) to form in the muscle and those can cause the pain we’re talking about.
How To Tell The Difference
It’s not a perfect test, but there are some general patterns that can help:
If it’s true sciatica (nerve-related), the pain usually travels down the back of the leg and often gets worse when you bend forward, like when you’re trying to touch your toes.
If it’s coming from the glute minimus, the pain is more likely to run down the side of the leg, flexion doesn’t cause the pain, and you can often reproduce it by pressing on the muscle.
How I Helped My Patient
We kept things pretty simple.
First, I worked directly on the trigger point in the glute minimus with manual therapy to calm it down.
Then we focused on strengthening the glute minimus and the muscles that support it. That included seated hip internal rotation and single leg RDLs.
We also added glute bridges to build strength in the glute max so the minimus didn’t have to carry as much of the load.
She did the exercises almost every day, and I saw her once a week to guide the process.
Each week, her symptoms improved. By the third week, the pain was gone.
What You Can Try
If this sounds like what you’re dealing with, you can do something very similar at home.
(Click on the links below to see how to perform the exercises)
Use a lacrosse ball on the glute minimus — 4 spots until pain decreases
Seated hip internal rotation — 3 sets of 10
Single leg RDL — 3 sets of 10/side
Glute bridges — 3 sets of 30 seconds
Doing the exercises above every day for about 4–6 weeks is often enough to calm things down and build better support around the hip.
When To Be Careful
If your pain is getting worse, feels constant, or comes with numbness or noticeable weakness, it’s worth getting it checked out.
The Bigger Takeaway
Not all leg pain is coming from your back.
And not everything that feels like sciatica actually is.
Sometimes it’s a muscle that’s been overworked for a long time. When you address that, things can improve much faster than you’d expect.
I hope this was helpful for you. If you have any questions about this or about your specific problem, you can always respond to these emails for help.
See you next week,

Dr. Matt Moreno, D.C., C.C.S.P.®
The Move More Minute
When you’re ready, here’s how I can help:
Start here: Joint Basics – Low Back & Hips
A structured, stability-first starting point so you can stop guessing what matters first.
Learn More About Joint BasicsNeed more help? Reply to this email
Tell me what you’re dealing with and I’ll try to help as much as possible.
Disclaimer: The information provided in this newsletter is for educational and informational purposes only and is not intended as a substitute for professional medical advice, diagnosis, or treatment. Always seek the advice of your physician, chiropractor, or other qualified healthcare provider with any questions you may have regarding a medical condition or before starting any new exercise program.
The exercises and suggestions provided are general recommendations and may not be suitable for everyone. If you experience pain, discomfort, or any concerning symptoms while performing these exercises (such as numbness, dizziness, or increased pain), stop immediately and consult a qualified healthcare professional.
Do not disregard professional medical advice or delay seeking it because of something you have read in this newsletter. The author, Move More Minute, and its affiliates assume no responsibility for injuries or issues that may arise from following the recommendations provided. By engaging with this content, you agree to do so at your own risk.
For personalized care or specific advice, please schedule an appointment with a qualified professional.

